 What Is Diabetes?
What Is Diabetes?
Diabetes is the condition when your blood glucose—also called blood sugar—is too high. Glucose is a form of sugar that your body uses for fuel. When you eat, most of the food is turned into glucose, which then enters the bloodstream and circulates around your body. An organ near the stomach called the pancreas produces insulin, which helps glucose get from your blood into your cells. Cells take up the glucose and turn it into energy. When you have diabetes, your body does not make enough insulin or the insulin produced does not function properly. As a result, glucose cannot get into the cells and begins to accumulate in the bloodstream.
Why is it Important for Teens to Know About Diabetes?
According to data published in 2006, over 150,000 young people under age 20 in the United States have diabetes. Among this group, about 80% are aged 10-19 years. As obesity rates in children continue to soar, diabetes is becoming more common in teens. Without proper treatment, diabetes puts an individual at higher risks of infection, nerve damage, heart disease, eye problem, and kidney failure.
What Are the Symptoms of Diabetes?
Symptoms vary from person to person. Some may show no symptoms at all. The most common are:
- Rapid weight loss
- Fatigue
- Increased thirst and urination
- Frequent hunger
- Blurred vision
- Slow healing wounds
- Tingling or numbness in feet
- Itchy skin
How is Diabetes Diagnosed?
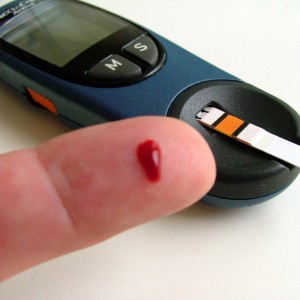
A blood glucose test can detect diabetes. A normal fasting blood glucose level is less than 100 mg/dl. Fasting means no food intake for at least 8 hours. A level between 100-125-mg/dl signals pre-diabetes. A fasting glucose of 126 mg/dl or above on two occasions confirm a diagnosis of diabetes. People diagnosed with diabetes can routinely monitor their glucose levels using a blood glucose meter. The device can be easily purchased at local pharmacies and provides a quick and convenient method for self-testing. Most insurance companies cover the meters and supplies.
What Are the Different Types of Diabetes?
There are 3 main types of diabetes:
- Type 1 Diabetes: People with type 1 diabetes make very little or no insulin. This type of diabetes usually starts in childhood or adolescence but may occur at any age. Type 1 diabetes can be managed by daily insulin injections, a diabetic meal plan, and regular exercise.
- Type 2 Diabetes: People with type 2 diabetes make some insulin but not enough, or their bodies fail to respond to the insulin produced. Type 2 diabetes used to occur primarily in adulthood, but now more and more teens are developing type 2 diabetes, especially if they are overweight. For people who are overweight, losing weight can improve the body’s ability to use its insulin. People with type 2 diabetes may also need to take diabetes pills or insulin injections to treat the condition.
- Gestational Diabetes: This type of diabetes appears during pregnancy and usually disappears after delivery. Many women with gestational diabetes develop type 2 diabetes later on in life. Gestational diabetes can often be controlled by diet alone.
Tips for Diabetic Meal Planning:
For people with diabetes, having a properly planned diet is a crucial step in managing the condition. Here are several principles for healthy eating:
- Eat regular meals: ideally 3 small meals with 1-2 healthy snacks daily.
- Include foods high in fiber, such as brown rice, oats, dried beans, whole grain breads and cereals, fresh fruits, and vegetables.
- Choose low-fat protein foods: lean meats, chicken breast, tofu, and egg white.
- Avoid high-sugar foods: candies, soda, syrup, jams, juices and desserts.
- Limit refined foods: white bread, white rice, jook (congee).
- Avoid high-cholesterol foods: egg yolk, shrimp, squid, and organ meats.
- Limit consumption of fast foods, fried foods, animal fats, and salty (high sodium) items.
Benefits of Exercise:
The benefits of exercise are endless. Besides helping to maintain a healthy weight, regular physical activities lower blood glucose levels, improve insulin sensitivity, strengthen your muscles and bones, and reduce your risk of other diseases. Combined with a healthy diet, routine exercise also helps to lower your need for insulin or diabetes medications. In fact, some people can manage their diabetes by diet and exercise alone.
Exercise Guidelines for People with Diabetes:
- Always consult your health care team before starting a new exercise program.
- Check blood glucose levels before and after a workout, to make sure your levels are neither too high nor too low. If glucose levels are too low (below 100 mg/dl) before a workout, have a snack and retest in 15 minutes. Find out from your health care provider what is the appropriate range of glucose levels for you.
- Ask your doctor whether you need to adjust your insulin dosage before exercising to prevent low blood sugar (hypoglycemia).
- Keep a source of fast acting carbohydrates (e.g., glucose tablets) on you in case blood glucose levels become too low during exercise.
- Wear comfortable shoes and breathable socks to prevent foot problems.
- Bring a water bottle with you. Dehydration can increase blood glucose levels and affect heart function.
- Warm up for 5-10 minutes and start with low-intensity activities.
- Spend 5-10 minutes to cool-down after exercise.
For More Information on Diabetes:
- Chinese Community Health Resource Center: http://cchrchealth.org/en/healthinfo/materials/diabetes.html
- Joslin’s Asian American Diabetes Initiative (AADI): http://aadi.joslin.org
- Juvenile Diabetes Research Foundation International: http://www.jdrf.org


